Efficient and accurate medical billing and credentialing services are crucial for the success of healthcare providers and organizations. From understanding their importance to exploring the benefits of national medical billing services and finding reliable options, we aim to empower you with the knowledge needed to navigate this vital aspect of healthcare management effectively. We will provide you with expert tips and insights on medical billing and credentialing services in 2023, helping you navigate the complexities of this essential aspect of healthcare management.

Medical billing is the process of submitting and processing healthcare claims to insurance companies or payers for reimbursement. It relies on accurate coding and documentation to ensure timely and maximum reimbursements. Credentialing involves verifying and assessing the qualifications, training, and expertise of healthcare providers. It includes obtaining and maintaining the necessary credentials, licenses, and certifications to practice in a specific field or with specific insurance networks.
For healthcare providers seeking to streamline their operations and focus on patient care, outsourcing medical billing and credentialing services offers several advantages. National medical billing services provide expertise, resources, and scalability, allowing healthcare professionals to enhance revenue cycles and improve overall efficiency. By outsourcing, providers can access specialized knowledge, stay compliant with evolving regulations, reduce administrative burdens, and increase revenue.
When searching for medical billing and credentialing services near you, it is crucial to consider several factors to ensure a seamless partnership. Look for service providers with a proven track record, extensive experience, and a comprehensive understanding of the intricacies of medical billing and credentialing. They should be well-versed in the latest coding systems (such as ICD-10 and CPT) and possess up-to-date knowledge of billing regulations.
In the modern era, technology plays a critical role in optimizing medical billing and credentialing processes. Leveraging electronic health record (EHR) systems, practice management software, and automated coding tools can streamline operations, reduce errors, and accelerate reimbursements. Automation also ensures compliance with regulations, minimizes paperwork, and enhances data security.
Healthcare providers must adhere to existing coding and billing requirements to avoid claim denials and payment delays. Review and educate your coding and billing team regularly to guarantee compliance with current standards. To reduce mistakes and optimize reimbursement, familiarise yourself with the programming system, modifier, and documentation updates.
Medical billing and credentialing performance must be monitored using key KPIs. Track claim acceptance, average reimbursement time, rejection rates, and accounts receivable turnover. These KPIs assist detect bottlenecks, optimize methods, and boost profitability and efficiency in operations.
Medical billing and credentialing services must comply with evolving regulations. Make that your service provider follows HIPAA, CMS, and payer-specific rules. Internal audits and comprehensive compliance programs reduce risks and protect patient data.
New trends and challenges: Medical billing and credentialing
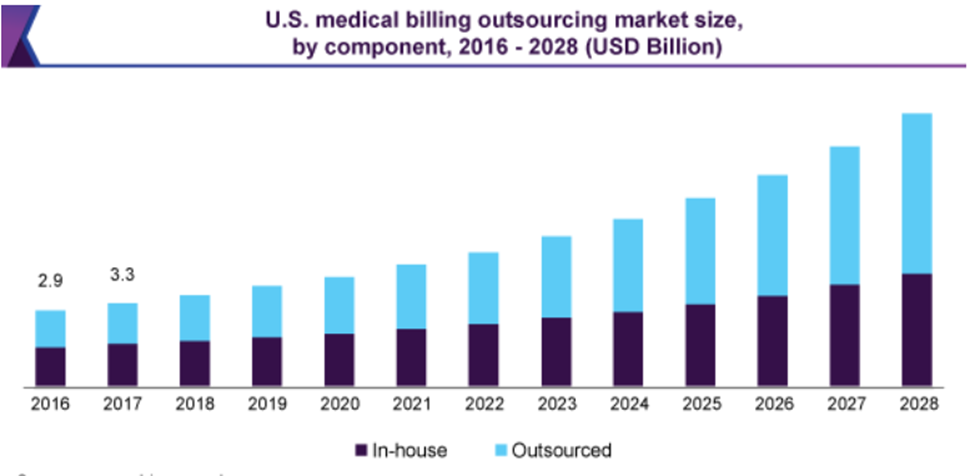
In 2023, there are some new trends and challenges that healthcare providers will need to be aware of when it comes to medical billing and credentialing. These include:
Insurance regulations are becoming more intricate, requiring healthcare providers to navigate complex billing requirements. Staying up-to-date with the latest regulations ensures accurate coding, proper documentation, and timely reimbursements.
The number of people with complicated medical disorders is increasing in the healthcare system. This creates difficulties in appropriately coding and billing for specialized treatments including services, necessitating the need for healthcare practitioners to guarantee sufficient documentation and coding correctness to prevent claim rejections.
Healthcare costs continue to expand, keeping pressure on providers to optimize their revenue cycles. Efficient medical billing and credentialing systems maximize payments while minimizing income loss, allowing providers to efficiently handle financial issues.
Credentialing and provider enrollment processes are affected by the shortage of qualified healthcare professionals. Maintaining a network of qualified providers requires efficient credentialing management by healthcare organizations.
With advances in electronic health records, artificial intelligence, and automation tools, medical billing, and credentialing are being transformed by a technological revolution. By embracing technology, providers can streamline processes, minimize errors, and improve efficiency, allowing them to focus more on patient care.
There is an increasing emphasis on quality of care and patient outcomes in the healthcare industry, which is reflected in value-based reimbursement models. To meet the changing reimbursement requirements, healthcare providers need to adapt their billing and credentialing practices.
Healthcare organizations face growing concerns about data security and privacy as electronic systems and patient data become more prevalent. Patients’ information must be safeguarded by providers adhering to HIPAA regulations and robust cybersecurity measures.
There are new complications with medical billing and credentialing due to the expansion of telehealth services. To guarantee proper billing and reimbursement, healthcare practitioners must be familiar with telehealth reimbursement rules and regulations.
To meet these challenges, healthcare providers need to be proactive in managing their medical billing and credentialing processes. Here are a few tips to help you get started:
Benefits of using medical billing and credentialing services

Conclusion
Mastering medical billing and credentialing services is essential for healthcare providers. Outsourcing these services offers benefits such as expertise, scalability, and increased revenue. Embracing automation, staying updated with coding guidelines, monitoring key performance indicators, and maintaining compliance is crucial. New trends and challenges include complex insurance regulations, patients with complex needs, rising healthcare costs, and a shortage of qualified professionals. Using medical billing and credentialing services brings accuracy, efficiency, reduced costs, improved cash flow, and compliance. Choose a reputable company with experience in your practice. By following these tips, healthcare providers can optimize revenue, streamline processes, and ensure success in 2023 and beyond.